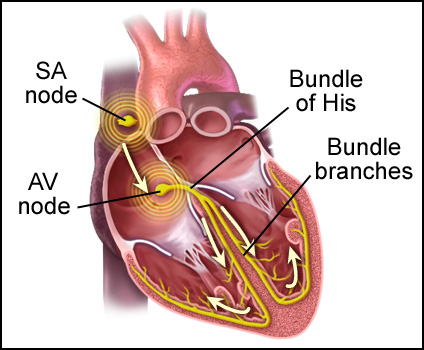
We acknowledge that certain medications can contribute to QT prolongation and the development of torsades de pointes. 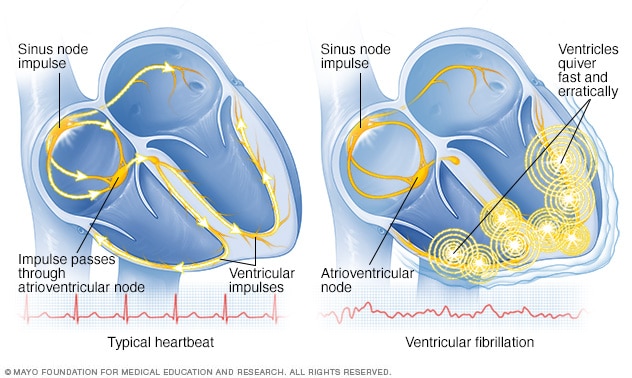
An acute coronary occlusion was ruled out with angiography and a lack of substrate for reentrant ventricular tachycardia by programmed stimulation. This is consistent with the studies described previously, which showed prolonged repolarization secondary to an abrupt reduction in heart rate after ablation. The heart rate was 52 bpm, compared to 103 bpm preprocedure, and the QTc prolonged to 559 ms, compared to 419 ms preprocedure ( Figure 1A and B). After ablation, atrial flutter was terminated and the patient’s rhythm reverted to sinus bradycardia. The patient had several risk factors described previously, including dilated cardiomyopathy and structural heart disease (mixed mitral valve disease, mild aortic stenosis). 5, 9, 10 Sudden death was exclusively seen in patients who had narrow QRS complex or right bundle branch block prior to AVJ ablation but not in patients with preexisting left bundle branch block. The presence of dilated cardiomyopathy, structural heart disease (particularly mitral stenosis, but also aortic stenosis and aortic regurgitation), New York Heart Association functional class greater than II, preprocedure ventricular arrhythmia, diabetes, and chronic obstructive pulmonary disease were all associated risk factors. The risk factors for sudden death after AVJ ablation and pacemaker insertion for AF have been investigated. Heart failure, hypokalemia, and female sex can prolong repolarization and also increase the risk of ventricular arrhythmias after ablation. Furthermore, an ECG at 6 months follow-up showed that the QTc remained normal at 423 ms ( Figure 3B). There was no recurrent syncope or arrhythmia at 1, 3, and 6 months follow-up (including 24-hour Holter monitor). An ECG 13 days after cardiac arrest demonstrated that the QTc was 408 ms ( Figure 3A). Serial daily ECGs after ablation identified that it took 48 hours for the QTc to shorten to 450 ms and 10 days to shorten to less than 440 ms. The patient was monitored on telemetry for 14 days post cardiac arrest and there was no recurrence of ventricular arrhythmia. The patient was hospitalized for 14 days after the cardiac arrest as a result of musculoskeletal injury secondary to cardiopulmonary resuscitation and a catheter-related urinary tract infection, as well as for further investigations, which included coronary angiography (which showed native coronary artery disease but patent bypass grafts) and an electrophysiology study (which failed to induce ventricular arrhythmia with programmed stimulation and up to 4 extrastimuli, without isoprenaline). A transthoracic echocardiogram done following cardiac arrest revealed stable cardiac structure and function with no new regional wall motion abnormalities. The blood chemistry revealed a pH of 7.35, potassium of 4.7mmol/L (normal range 3.2–5.0 mmol/L), and magnesium 0.91 mmol/L (normal range 0.70–1.10 mmol/L). 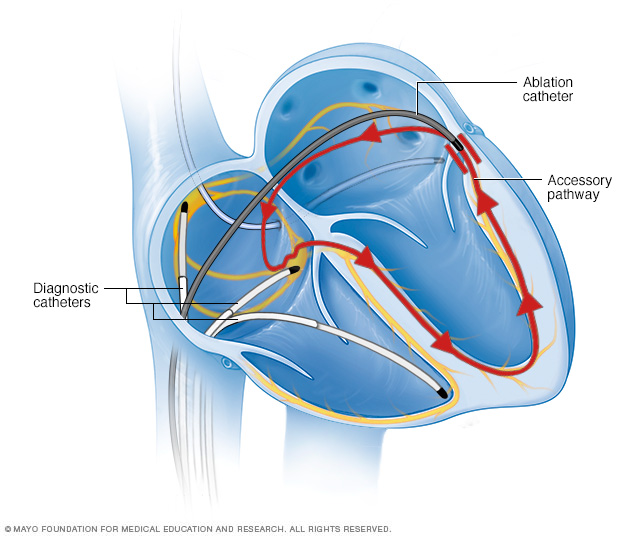
The average monitored heart rate prior to the ventricular arrhythmia was between 60 and 65 bpm. Seven hours postprocedure, the patient developed polymorphic ventricular tachycardia, which was terminated after 2 minutes with a single 200 J biphasic DC shock ( Figure 2). The patient’s regular medications included aspirin, dabigatran, perindopril, metoprolol, digoxin, isosorbide mononitrate, rosuvastatin and pantoprazole. Following anticoagulation with dabigatran 150 mg twice a day and a subsequent transesophageal echocardiogram confirming resolution of the atrial thrombus, the decision was made to proceed to catheter ablation. Two attempts at transesophageal echocardiogram with cardioversion were aborted owing to thrombus in the atrial appendage despite oral anticoagulation with apixaban 5 mg twice a day or warfarin. Over recent years the patient experienced episodes of paroxysmal atrial flutter, with a persistent episode occurring 12 months prior to referral to our hospital. Eighteen years prior the patient underwent coronary artery bypass grafting and mitral valve repair. A 75-year-old woman with a history of coronary artery disease, heart failure, and persistent and inadequately rate-controlled atrial flutter was referred for catheter ablation.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
